Public policy, often judged by its intentions, sometimes fails to deliver the desired results. The Affordable Care Act is a prime example. It was presented as a reform intended to lower costs, expand access, and introduce competition into the healthcare marketplace. However, it produced a system in which costs continued to rise, choices narrowed, and the most significant financial gains went not to patients but to the insurance companies set at the center of the law’s design.
President Trump has now challenged the fundamental structure of that system. He argues that the ACA’s subsidies should no longer be paid to insurance companies but should be paid directly to the American people. Whatever one thinks of Trump personally, his proposal forces a question that Washington has avoided for more than a decade: Why should billions of taxpayer dollars pass through corporate accounts before reaching the citizens the law is supposedly designed to help?
This is not a question of sentiment or partisan emotion. It is a question of incentives.
The ACA’s Incentives: A System Built Around Insurers
The ACA’s core mechanism is straightforward: individuals who qualify for subsidies do not receive the money. The government sends those subsidies directly to insurance companies. In practice, this means insurers are guaranteed federal revenue regardless of whether they innovate, reduce costs, or deliver higher quality coverage.
The results speak for themselves. Independent analysis shows that the weighted average stock price of major health insurance companies has risen more than 1,032 percent since the ACA was enacted in 2010. Premiums for ACA plans, meanwhile, are projected to rise again in 2026—double-digit increases in many states—despite more than a decade of promises that the law would control costs.
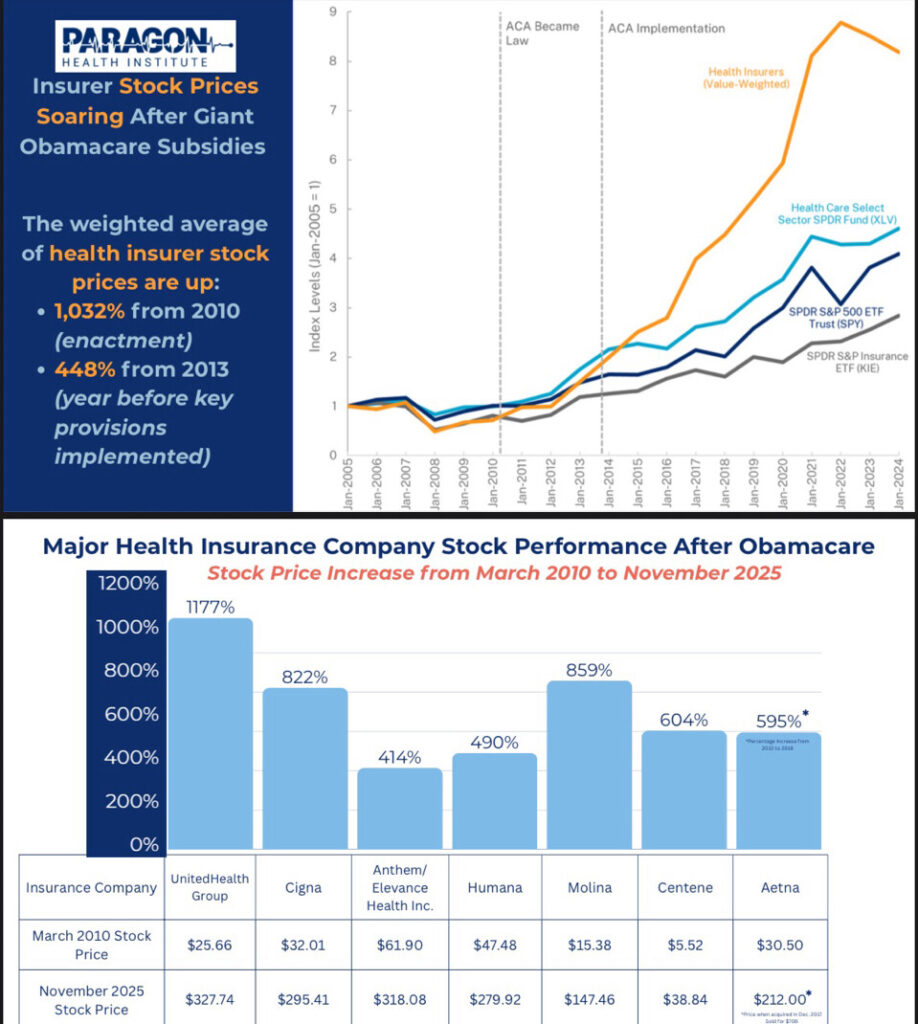
If a law produces one group of clear financial winners and another group of increasingly burdened consumers, the incentives are revealing. The ACA successfully expanded coverage for some Americans, but it did so by embedding private insurance companies deeper into the public financing structure. The marketplace did not become more competitive; it became more dependent on federal subsidies.
The Clarification Politicians Avoid
As with most major policy debates, misinformation thrives when political power is at stake. So a basic clarification is necessary: Trump’s proposal does not alter Medicaid, Medicare, union-negotiated insurance plans, employer-sponsored coverage, VA benefits, or TRICARE. Seniors keep their benefits. Low-income families keep theirs. Union workers and employees retain their existing plans.
The only component under scrutiny is the ACA’s subsidy design—the part in which the federal government pays insurers rather than individuals.
The significance of that clarification is substantial. This discussion does not touch Americans who rely on non-ACA coverage. The debate centers solely on whether ACA marketplace subsidies should continue flowing to corporations or be redirected to citizens.
The Insurance Companies Influence Over Congress
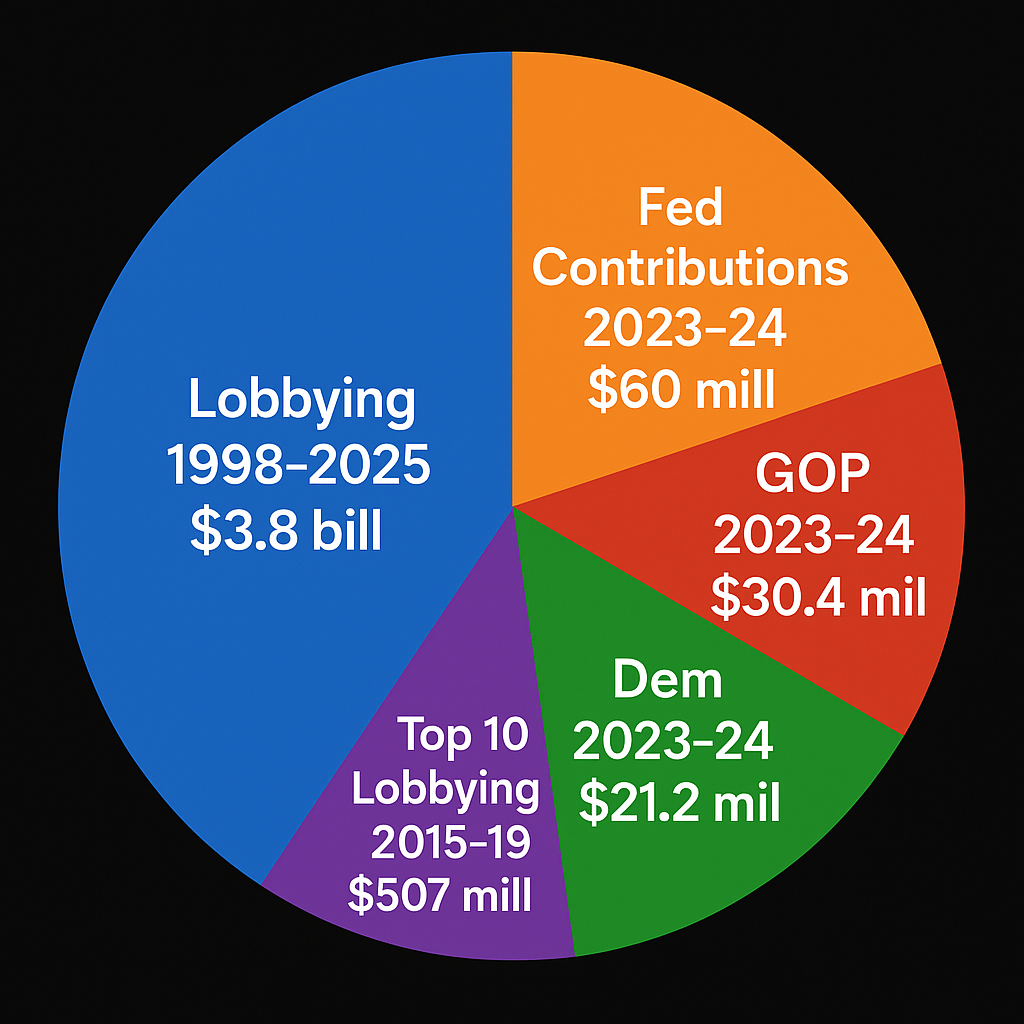
Insurance companies exert enormous influence over Congress, and the scale of their political spending makes that influence impossible to ignore. Over the last two decades, the insurance industry has spent nearly $3.8 billion on lobbying—an amount that guarantees access few ordinary citizens will ever have. In the 2023–24 election cycle alone, insurers poured more than $60 million into federal campaign contributions, directing about $30.4 million to Republicans and $21.2 million to Democrats, ensuring both parties remain responsive to industry interests. This is not new. Between 2015 and 2019, ten of the largest insurance and healthcare provider organizations spent more than $507 million lobbying Congress, while four major insurers spent $8.7 million on state-level campaigns in just a three-year window. These sums are not charity; they are strategic investments designed to preserve a system where guaranteed federal subsidies flow to insurers first and consumers last. When corporations with this level of financial power shape the rules, it becomes far easier to maintain the status quo—and far harder for meaningful reform to emerge.
Political Incentives and the Resistance to Change
The most notable feature of the current debate is not the complexity of the proposal but the intensity of the resistance. The insurance lobby benefits enormously from the existing structure. Pharmaceutical companies benefit from the lack of downward price pressure. And both political parties receive substantial financial support from the broader healthcare industry.
It is therefore not surprising that structural reform—particularly reform that redirects federal dollars away from insurers—is met with bipartisan discomfort. The status quo is politically profitable even if it is economically inefficient.
Policy must eventually be judged by outcomes, not promises. If premiums climb, if deductibles rise, and if the most significant financial gains appear on corporate balance sheets rather than household budgets, then the system is not serving the public interest.
Why The Free Market is Essential in Healthcare
Trump claims that redirecting subsidy dollars to individuals would create a genuine open market in which insurers compete for customers. Critics warn that destabilizing the ACA’s structure could reduce protections for those with pre-existing conditions or increase volatility in the risk pool. Both arguments have merit, but they rest on very different assumptions about human behavior and institutional incentives.
The ACA model assumes that centralized management and guaranteed subsidies produce stability. The U.S. healthcare economy since 2010 suggests otherwise. Guaranteed federal payments reduced the pressure on insurers to innovate or minimize costs, contributing to rising premiums and a consolidation of insurance providers in many states. A marketplace with minimal competition is not a marketplace at all.
Redirecting funds to individuals would reverse those incentives. It may not solve every structural problem in American healthcare—no single reform could—but it corrects a fundamental flaw: the absence of consumer power, offering a hopeful vision for the future of healthcare.
The Question Washington Can No Longer Ignore
A functioning free market is essential in healthcare because it restores the one force the current system lacks: accountability to the consumer. When insurance companies receive guaranteed federal subsidies regardless of cost or performance, they have no incentive to innovate, lower prices, or improve the quality of coverage. A free market reverses that dynamic. It forces insurers to compete for customers rather than lobby for government dollars. Prices fall when companies cannot rely on subsidies to survive, and quality rises when consumers—not bureaucracies—decide who deserves their business. Without a free market, healthcare becomes a protected cartel in which corporations profit while families pay more each year. With a free market, the power shifts back to the individual, which is the foundation of any system that claims to serve the public rather than the politically connected
The Question Washington Can No Longer Ignore
The real issue is not whether the ACA helped some people—it did. The real problem is that it did so through a mechanism that enriched insurers far faster than it helped patients, left premiums rising well above wage growth, and failed to deliver the competition it promised.
Trump’s proposal forces a long-overdue examination of whether healthcare dollars should belong to the people who need care or to the corporations that administer it.
The most important public policy questions are often the simplest. In this case, the question is: Who should control the money? It’s a question that demands our attention and thoughtful consideration.
Politicians may continue avoiding that question. Interest groups may continue lobbying to prevent it from being answered. But the reality remains: the ACA’s financial structure is a policy choice, not an inevitability.
And now, for the first time in more than a decade, that choice is finally being challenged, underscoring the urgency of the issue at hand.
References
1. Paragon Health Institute.
“Health Insurer Profits Under the Affordable Care Act.”
Shows that the weighted average stock price of major U.S. health insurers increased 1,032% from 2010 to 2025.
https://paragoninstitute.org
2. OpenSecrets – Center for Responsive Politics.
“Insurance Industry: Lobbying, 1998–2025.”
Documents approximately $3.8 billion in lobbying expenditures by the insurance industry between 1998 and 2025.
https://www.opensecrets.org/industries/lobbying?ind=F09
3. InsuranceNewsNet.
“Insurers & Trade Groups Seek Influence via Donations in Divisive Election.”
Details $60 million in federal political contributions from the insurance industry during the 2023–24 cycle, with $30.4 million to Republicans and $21.2 million to Democrats.
https://insurancenewsnet.com/innarticle/insurers-trade-groups-seek-influence-via-donations-in-divisive-election
4. FollowTheMoney.org – National Institute on Money in Politics.
“Health Insurance Companies Give Healthy Donations to Political Campaigns.”
Analyzes state-level donations, including $8.7 million from major insurers (WellPoint, UnitedHealth, Humana, Aetna) between 2005–2008.
https://followthemoney.org
5. AMA Journal of Ethics / PMC.
“Influence of Health Care Industry Spending on Policy: Federal Lobbying by Health Systems and Insurers (2015–2019).”
Reports $507 million in lobbying spending from the top 10 healthcare and insurance organizations during 2015–19.
https://pmc.ncbi.nlm.nih.gov/articles/PMC8694571
6. Politico.
“Obamacare Could Collapse Under Trump’s New Plan, Policy Experts Say.”
Explains concerns about how redirecting subsidies could impact ACA marketplaces but confirms the ACA’s structural reliance on insurance company subsidies.
https://politico.com
7. Kaiser Family Foundation (KFF).
“Marketplace Premium Trends and Insurer Financial Performance.”
Provides data on premium increases and insurer profitability under the ACA.
https://kff.org
8. Congressional Research Service (CRS).
“The Affordable Care Act: A Summary of Financial Structure and Subsidies.”
Explains how premium subsidies are paid directly to insurance companies rather than individuals.
https://crsreports.congress.gov














